The Gap. Part III: Rebuild.
What I would do if I were in the room.
I owe you an apology, and I’m not going to give you one. I am still showing up. Sometimes weaker. Sometimes wiped out. But I always show up.
Part II ran nearly a month ago. Part III was supposed to follow within two weeks. Instead I got sick again, landed back in court navigating proceedings, and spent most of the last few weeks doing exactly what this series is about: navigating a system that has no answer for someone like me, while keeping my head above water, growing businesses, and managing a medical situation that does not stay still.
That is not a digression from the story. That is the story.
Every delay in this series is a receipt. Every missed deadline is what the gap costs a person in real time. I am not writing about healthcare from a policy desk. I am writing about it from inside it. Between migraines, impaired vision, antibiotics, and court hearings. My eight-month wait for the neuro-ophthalmologist came up this week. I had to put it on hold until my new expensive subpar HMO plan kicks in at the beginning of May.
Over the next month there will be a lot happening. A big day in court. An MRI and more imaging. Several medical appointments I can no longer defer.
So here we are. Part III. The rebuild.
Not a rant. A framework.
What I Promised You
In Part I, I laid out three paths that are actually on the table. Not the fake binary everyone argues about on cable news. The three real ones.
Universal coverage — with all the wait lists that come with it.
True market competition — eliminating state lines, letting companies compete for your business nationwide, and forcing the math to actually work.
Eliminate the fraud and corruption — bleeding the system dry before anyone sees a dime of actual care.
I said all three were better than what we have now. I still believe that.
But after years of living this, running the numbers, and reading what every other country has actually tried, I am going to tell you a harder truth.
Half a lung removed. Every respiratory infection since is a potential emergency. Every imaging delay is a gamble. This is not an academic exercise for me. This is the environment I live in.
None of them works alone.
First, The Part Nobody Says Out Loud
Before we go anywhere else, one fact has to land first.
The United States has the best medical talent in the world. That is not a patriotic talking point. That is a global fact.
When a head of state, a foreign minister, or a Saudi prince needs a major procedure, they do not get on a plane to Toronto. They do not fly to London. They fly to Cleveland, Houston, Baltimore, Rochester, New York, DC, or Boston. Walk the halls of George Washington Hospital or Georgetown University Hospital in DC. Walk into the Cleveland Clinic. The Mayo Clinic. Mass General. Johns Hopkins. MD Anderson. You will hear ten languages before you reach the elevator. People fly across oceans to be treated here because the surgical expertise, the research, the equipment, and the outcomes in these hospitals are still unmatched anywhere on earth.
So when someone tells you “the American healthcare system is broken,” that statement needs a qualifier.
The care is not broken. The delivery, pricing, and access model around the care is broken.
Keep that distinction in mind for the rest of this piece. Because every reform conversation in this country goes off the rails within five minutes when someone conflates the two. The people who want to tear the whole system down and rebuild it on a Canadian or British model are not just attacking the billing structure. They are risking the part of American medicine that actually works. The part that saves people the rest of the world cannot save.
We do not need to replace our medical system. We need to replace the financial structure wrapped around it.
Now. The rest.
Universal Coverage Is Not What You Think It Is
People on one side of this argument talk about universal coverage like it solves the problem. It does not. It solves a different problem than the one I am living.
Canada has universal coverage. In 2025, the median wait time from GP referral to actual treatment across twelve specialties was 28.6 weeks. That is the second-longest wait ever recorded in the country’s history. Patients in New Brunswick waited over a year. Across the country, an estimated 1.4 million Canadians were sitting on a waitlist for a procedure.
The UK has universal coverage. The NHS has not met its own four-hour emergency room standard in over a decade. Its urgent cancer referral benchmark is 28 days. Its non-urgent specialist standard is measured in months.
And before anyone says “that’s other countries,” we already run universal systems inside the United States. Medicare. Medicaid. The VA.
The VA’s own published standard for specialty care is 28 days. After that, veterans are eligible to seek care in the community on the government’s dime. That standard exists precisely because the VA could not meet its own access goals for decades. In 2014, a Phoenix audit revealed over 1,700 patients had been placed on secret waitlists. Some died before being seen. That was not a foreign country. That was our universal system.
I already told you I waited months for a specialist in the United States on an urgent list. I am now at eight months, still waiting, paying private market premiums that consume a shocking percentage of my income. Nobody gets to tell me universal coverage would have saved me time. It would have saved me money. Those are not equivalent.
Universal coverage solves the bankruptcy question. It does not solve the access question.
When your head is throbbing and your doctor ordered the imaging and you cannot afford it, you do not care whether the bill is coming from a private insurer or a government program. You care whether you can get the scan.
Universal coverage answers the bill. It does not answer the scan.
So the people who argue that it is the single silver bullet are wrong. And the people who argue that it is communism are also wrong. It is a tool. It handles one specific problem very well. It does not handle the others.
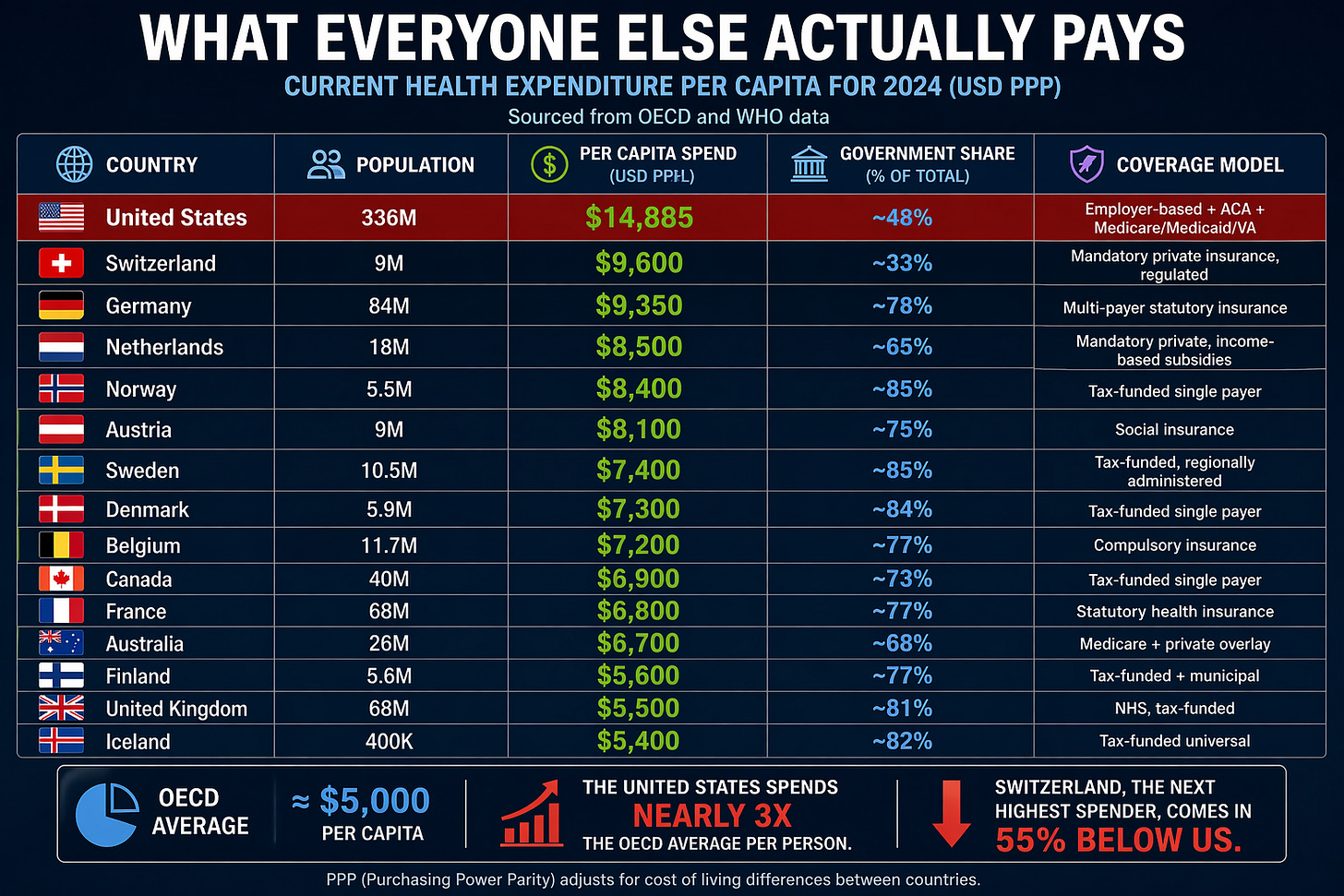
What Everyone Else Actually Pays
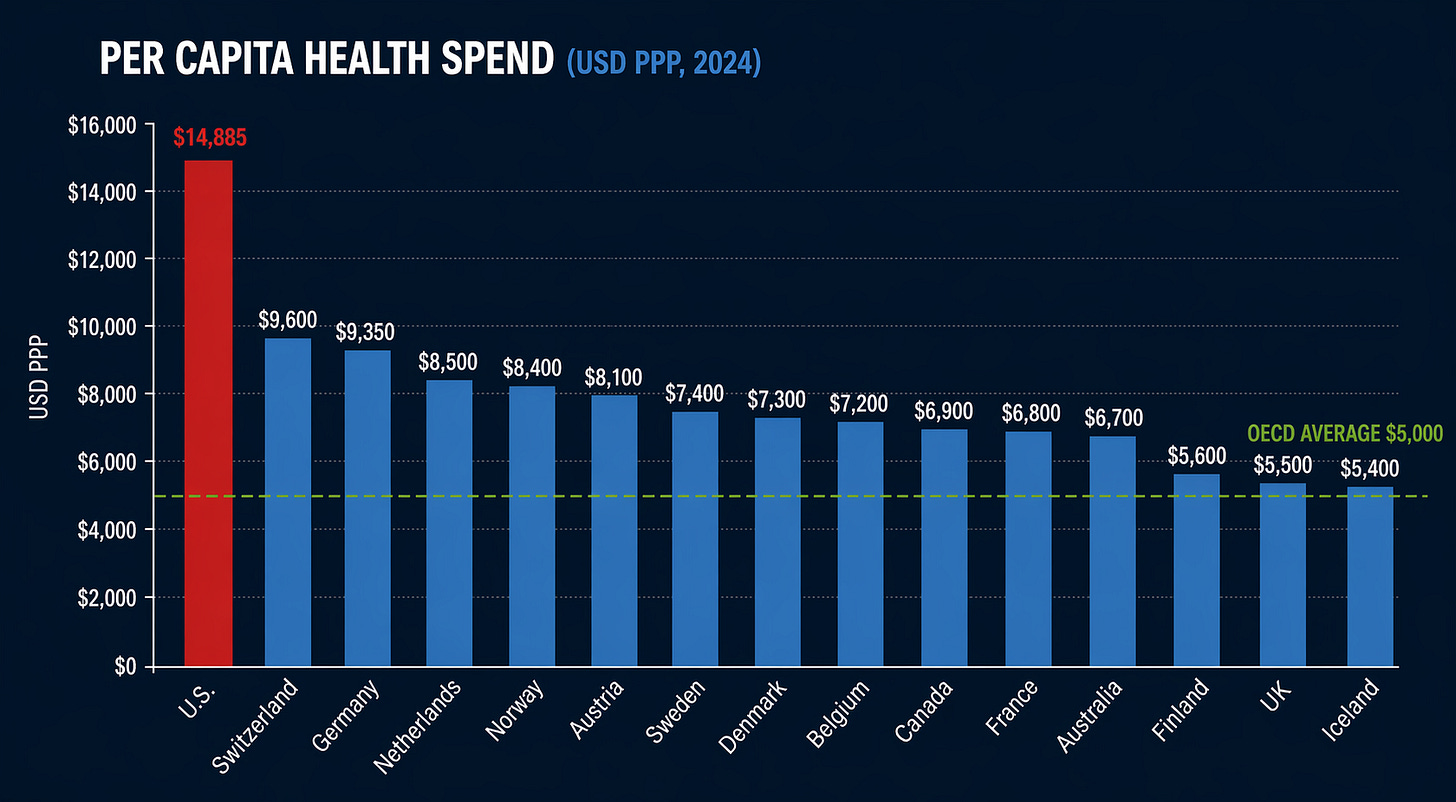
Here is a side-by-side picture rarely shown clearly. What every major country spends per person on healthcare, what portion their government covers, and what their citizens actually get for that money.
Numbers below are current health expenditure per capita for 2024, sourced from OECD and WHO data.
The OECD average is approximately $5,000 per capita. The United States spends nearly three times the OECD average per person. Switzerland, the next highest spender, comes in 55% below us.
And here is the part that matters.
Life expectancy in the United States is the lowest of every country on that list.
We pay the most. We cover the fewest. We wait the longest for imaging many Americans cannot even afford. Our infant mortality is higher than every country in the table. Our maternal mortality is worse than every country in the table. Our rates of chronic disease are worse than every country in the table.
More spending does not buy better outcomes. It buys a larger billing apparatus.
Every country on that list solved a problem we have not. They built a financing structure that aligns what you pay with what you receive. They did not build a better medical system than ours. They built a better payment system around their medical system.
That distinction is the entire argument.
The Market Answer Was Already Legal. Nobody Used It.
This is the part nobody on either side wants to talk about.
When politicians campaign on “letting insurance compete across state lines,” they are selling you a solution that has already existed in federal law for more than a decade.
Section 1333 of the Affordable Care Act specifically authorizes interstate healthcare compacts. Two or more states can agree to let insurers licensed in one sell policies in the others. The mechanism exists. The legal framework exists. It has existed since 2014.
At least nine states have passed laws authorizing themselves to enter such a compact. Georgia. Maine. Kentucky. Rhode Island. Wyoming. Others.
Number of compacts that have actually formed: zero.
Number of policies ever sold across state lines through this mechanism: zero.
Read that again. For over a decade, states have had the legal authority to do what politicians keep promising they will fight to make legal. And none of them did it. Not a single one.
Why?
Because the economics do not work the way the slogan works. Insurance premiums are not primarily driven by state regulations. They are driven by local healthcare costs. When a hospital in Florida charges four times what a hospital in Iowa charges for the same procedure, an insurance company from Iowa cannot “sell cheap insurance in Florida” because the insurance company still has to pay the Florida hospital the Florida price.
What actually ends up happening under unrestricted interstate sales, according to every regulator who has studied it, is this. Insurance companies relocate to whichever state has the weakest consumer protections. They write policies that exclude the conditions that cost the most. They sell those policies into other states by marketing to healthy people. The healthy people save a little money. The sick people get priced out. The state-level consumer protections that took decades to build get hollowed out.
That is what the industry itself told CMS when asked for comment. Five major insurers said a new federal mechanism was unnecessary and that interstate sales would not meaningfully lower premiums. Consumer advocacy groups including the American Heart Association and the American Diabetes Association agreed, from the opposite direction.
So when you hear “we need to let insurance compete across state lines,” understand what is actually being proposed. It is not more competition. It is regulatory arbitrage. It is allowing companies to choose their regulator.
I know what that looks like because I watched banks do the identical move in the early 2000s. That did not end well.
Market competition is good. But competition in healthcare requires what we have not had in fifty years. Real price transparency. Hospitals publishing their actual costs. Providers competing on quality and outcomes, not on which billing code they can get away with. A market where the person paying the bill can see what they are paying for before the service is delivered.
Interstate sales without price transparency is not competition. It is a regulatory shell game.
So option two, by itself, also fails.
Now Let’s Talk About the Fraud. And the Real Number.
This is the option nobody wants to talk about because it implicates everyone.
In June of 2025, the Department of Justice announced the single largest healthcare fraud takedown in American history.
324 defendants charged.
96 of them licensed medical professionals: doctors, nurse practitioners, pharmacists.
Over $14.6 billion in fraudulent billings in a single coordinated enforcement action.
More than double the previous record.
Inside that takedown was an operation called Gold Rush. A transnational criminal organization bought dozens of medical supply companies across the United States using foreign straw owners. They then submitted $10.6 billion in fraudulent Medicare claims for urinary catheters and durable medical equipment.
The beneficiary identities on those claims were stolen from over one million Americans.
One. Million. Americans had their Medicare identities used in a single fraud scheme.
That is not waste. That is not abuse. That is organized theft on a scale most people cannot picture, from a program funded entirely by taxpayers, targeting the elderly and disabled specifically because they are the most vulnerable.
What We Prosecute. What We Estimate. What It Actually Is.
Since the DOJ’s Healthcare Fraud Strike Force launched in 2007, it has charged more than 6,200 defendants who collectively billed federal programs and private insurers over $45 billion.
That is the prosecuted fraud. The fraud that was caught, indicted, and resolved.
The estimated fraud is a different number entirely.
The Government Accountability Office reports that Medicare and Medicaid combined generated over $100 billion in improper payments in fiscal year 2023. That was roughly 43 percent of the entire federal government’s improper payment total for the year. For fiscal year 2025, Medicare Fee-for-Service improper payments alone ran in the tens of billions. Medicaid improper payments that year ran $37.4 billion.
Now. CMS will correctly point out that “improper payments” is not the same as “fraud.” Most of those improper payments are classified as improper because of missing documentation, not because someone intentionally stole from the program. That distinction matters.
But the Senior Medicare Patrol, the federally-funded program dedicated to educating beneficiaries about fraud, estimates that Medicare alone loses roughly $60 billion per year to actual fraud, errors, and abuse.
Add Medicaid. Add private insurance fraud. Add the fraud that never gets flagged because the billing codes line up cleanly enough to pass an automated check.
Credible estimates for the total annual cost of healthcare fraud in the United States, across public and private payers combined, range from $100 billion to $300 billion per year.
Let that number sit.
What that actually means.
If the real number is $200 billion a year, right in the middle of the credible range, then over a decade, that is two trillion dollars stolen from American healthcare.
Two trillion dollars would fund universal catastrophic coverage for every uninsured American multiple times over. It would pay down the entirety of every red state’s Medicaid expansion concerns. It would fund the VA’s technology modernization, the CMS payment integrity overhaul, and real-time claims verification infrastructure with money left over.
That is the money that is missing. Not from a budget fight on the Hill. From theft. Some of it organized. Some of it opportunistic. All of it absorbed silently by a system that treats loss as a cost of doing business.
The fraud is not a rounding error. The fraud is roughly the size of the problem everyone keeps saying is unsolvable.
When you have a multi-trillion-dollar flow of money moving through a byzantine billing apparatus with no real-time oversight, and when the people who catch it catch it years after the money is gone, you have not built a healthcare system. You have built a laundering operation with a hospital attached.
CMS said it prevented another $4 billion in improper payments ahead of the 2025 takedown using AI-powered analytics. That is good. It is also the equivalent of installing a better lock on a building that has been robbed every day for twenty years.
You cannot fix premiums in a system that is bleeding this much money in fraud. You cannot fund universal anything in a system that cannot tell which claims are real. You cannot have market competition in a system where fake companies bill for services that never happened and collect real money before anyone notices.
Fix the fraud or nothing else matters. That is not hyperbole. That is math.
A Quick Word on Obamacare
Before I go further, one thing has to be said out loud, because the entire national conversation about healthcare is broken by people using these terms interchangeably when they are not the same thing.
Medicaid is not Obamacare.
Medicare is not Obamacare.
The VA is not Obamacare.
These are four different programs, with four different histories, serving four different populations. Confusing them is not a small mistake. It is the thing that makes this entire debate incoherent, and it benefits the people who prefer the confusion.
Medicare started in 1965. It is a federal program for Americans 65 and older, funded through payroll taxes. It predates Obama by 43 years.
Medicaid also started in 1965. It is a joint federal-state program for low-income Americans. It has existed for 60 years. The ACA expanded eligibility in participating states in 2014, but Medicaid itself was not created by Obamacare. People were on Medicaid for generations before.
The VA started in 1946. It is a separate federal system serving veterans, with its own hospitals and providers.
Obamacare, formally the Affordable Care Act, is primarily about the individual insurance market. The marketplace at healthcare.gov. The premium subsidies. The rules preventing denial for preexisting conditions. The essential benefit requirements. It is a set of rules and subsidies layered on top of private insurance for the people who do not have coverage through an employer or one of the programs above.
That distinction matters right now because of something I have been hearing a lot lately.
“Obamacare doesn’t seem so bad anymore.”
It is usually said by people who were on Medicaid for years and have recently aged off, earned too much to qualify, or had some other change in status drop them into the individual market for the first time in their adult lives. They thought they were on Obamacare the whole time. They were not. They were on Medicaid, a program that has existed since 1965, which gave them coverage at low or no cost relative to the individual market.
Now that they are in the actual individual market, the one that the ACA governs, they are seeing the real price of insurance in this country for the first time. And they are reacting accordingly.
They are not wrong to notice what the individual market looks like. It is brutal. The premiums are crushing. The deductibles are higher than most people’s savings. The networks are narrow. The process of getting a claim paid is a part-time job.
What those voices are missing is that the individual market has looked like this for a long time. Small business owners, contractors, self-employed professionals, independent workers. We have been living in it for over a decade. The ACA changed who could access coverage. It did not change what the coverage costs or what it feels like to use.
Obamacare did not break the individual market. It moved more people into a market that was already broken.
This is the part of the conversation where politics has to step back and math has to step forward. The financial structure of the ACA was never sustainable on its own. It required enhanced subsidies, expanded Medicaid, and constant federal backfill to paper over the underlying cost problem. When any one of those pillars moved, whether subsidies expiring, a state refusing expansion, or federal matching rates shifting, the cracks showed up fast.
The people just now entering the individual market are experiencing what Part I laid out in full. The 94% of income consumed by a premium. The three-month wait for imaging. The coverage that doesn’t actually cover you until you have paid thousands out of pocket.
Their reaction is real. Their math is accurate. The system is crushing them.
But the system was crushing the rest of us before they got here. That is not a political point. That is chronology.
When more people feel the weight, more people are finally motivated to fix it. That is the opportunity in the moment.
The Hybrid
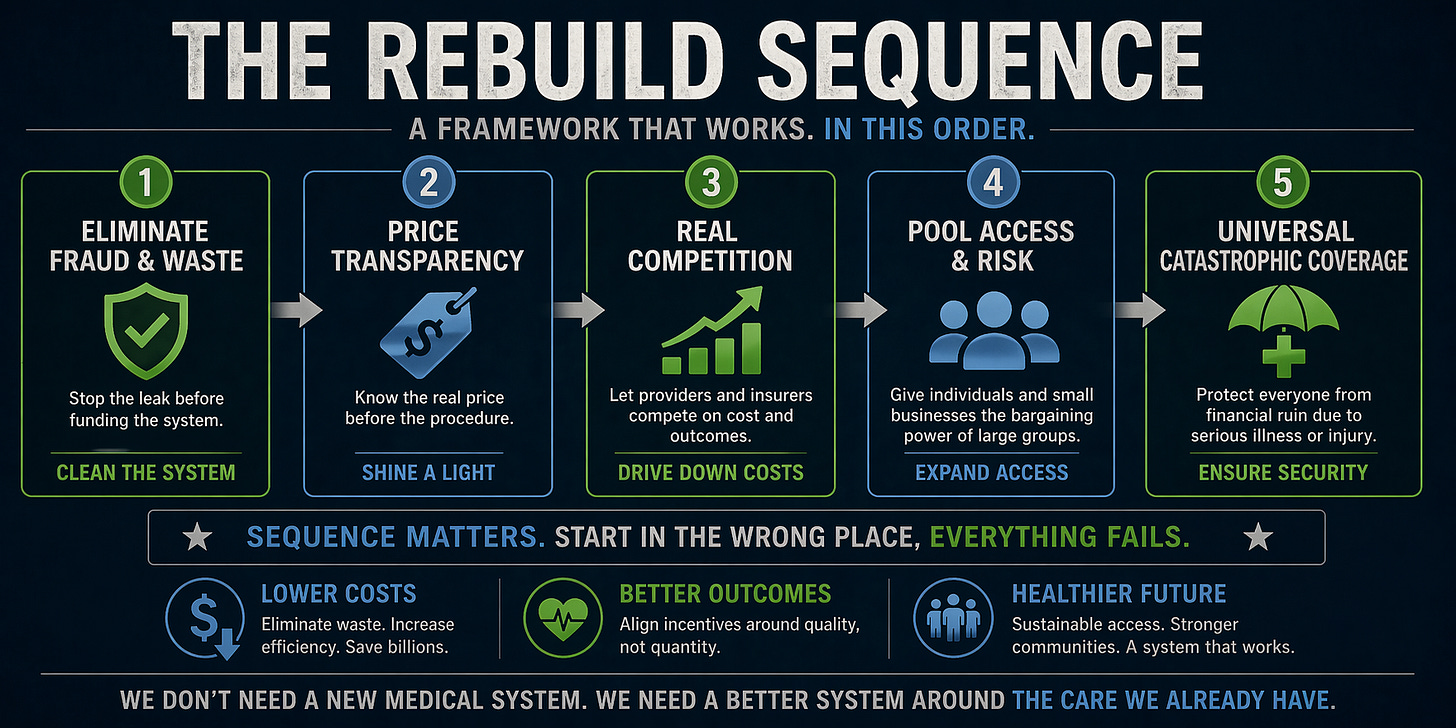
So if none of the three options works alone, what does?
They have to be sequenced. And they have to be built in a specific order, because each step depends on the one before it.
First: Eliminate the fraud. Before anything else.
Not as an eventual goal. As a precondition for every other reform.
You cannot rebuild a system with this much money leaking out of it. The 2025 Fusion Center, real-time data analytics, the expansion of whistleblower rewards under FinCEN, the AI-powered detection. All of it is a start. But the start is not the finish. The finish is a healthcare payment system where every claim is verified before it is paid, not audited two years after the money is gone.
That is a technology problem. We have the technology. What we have not had is the political will.
Until that is fixed, every dollar you put into the system, public or private, is funding both care and the people stealing from care. You cannot separate them with policy. You have to separate them with enforcement.
Second: Mandate real price transparency.
Not the kind hospitals claim to have now with machine-readable files buried four pages deep on websites nobody can navigate. Real transparency. The procedure you need. The price it costs. The same price for everyone. Published. Publicly. Before the service is delivered.
Without this, market competition is a fiction. You cannot choose the cheaper option if you do not know what anything costs until the bill arrives. Right now, you do not get to be a consumer in healthcare. You get to be a patient. A patient signs forms, gets procedures, and finds out months later what it cost. A consumer sees the price before the purchase.
Until we are consumers, there is no market.
Third: Allow genuine interstate competition, within a federal regulatory floor.
This is where I disagree with the purists on both sides.
Unrestricted interstate sales is the race to the bottom the regulators warned about. But a federal regulatory floor combined with real interstate competition is a different proposition entirely. It lets insurers compete on price, network strength, and administrative efficiency. It keeps them from competing on how successfully they can exclude sick people from coverage.
The ACA tried to create this framework and nobody used it because the mechanism was structured poorly. Redesign it. Keep the essential benefit floor. Kill the state-by-state fragmentation. Let real national carriers emerge.
There are 36 million small businesses in America. 30 million of them are one person. Another 5 million have fewer than 100 employees. Together they create 9 out of every 10 net new jobs in this country and account for nearly half of all private sector employment.
Fourth: Let solopreneurs pool like employers do.
This is the piece I have been living and the piece my industry has been living for twenty plus years.
Small businesses with employees have their own version of this problem, and they need their own fix. This section is about the 30 million Americans who are the business and the workforce at the same time.
The labor market has changed. The old fix for this, reclassifying gig workers as W-2 employees, no longer matches reality. The hairstylist renting her own chair is not being exploited by a misclassified employer. She is her own business. So is the dog walker with an LLC. The handyman with a truck and three regular clients. The graphic designer with a Shopify site and a subscription to Adobe. The accountant running her practice from her kitchen table at 2 a.m.
They did not get tricked into self-employment. Most of them chose it. They want the flexibility. They want to own their book of business. They are not asking to go back to a corporate job.
What they are paying for that freedom is brutal. The individual insurance market charges a solopreneur roughly three times what the same coverage costs inside an employer group plan. That premium is not based on risk. It is based on pool size. A single person buying insurance has no leverage. A company with 500 employees has enormous leverage. The entire pricing difference comes down to whether you have a crowd to stand inside.
Here is the fix.
One national pool. Every self-employed American in one place.
Not fragmented by industry. Not fragmented by state. Not fragmented by guild membership or trade affiliation. One federally chartered pool that any self-employed American can buy into, on the same terms as any other member.
Thirty million self-employed Americans in a single pool is the largest, most diverse, and most stable risk configuration in the country. Larger than any Fortune 500 employer plan. Larger than most state Medicaid programs. A pool that size does not need industry-specific underwriting, because the numbers average out faster and more predictably at scale than they do in any smaller subset. The 25-year-old freelance designer and the 58-year-old independent consultant and the 42-year-old contractor and the 35-year-old yoga instructor all stand in the same crowd, and the crowd is big enough to price them fairly.
Verification is simple, and the technology to do it already exists.
Leverage a federal self-employment verification portal. Think of it as an E-Verify system for the self-employed. Upload your documentation. AI does the first pass, cross-referencing against IRS records, Secretary of State business filings, payment processor data, and insurance carrier databases. Verification returns in minutes, not months.
Any one of the following confirms eligibility:
Prior-year tax filings showing Schedule C income, 1099 earnings, LLC distributions, or S-corp K-1s.
Current pay records. Client invoices, ACH deposits, Stripe statements, Square reports, PayPal business records, platform-issued 1099-NECs from Uber, DoorDash, Rover, TaskRabbit, or similar.
Active occupation-appropriate business insurance. Professional liability, general liability, errors and omissions, bonding. If you are running a real business, you are already carrying coverage your clients or landlord require.
None of this is theoretical. E-Verify has processed employment eligibility for 30 years. ID.me handles identity verification for the IRS, VA, and Social Security Administration every day. The federal government already uses AI-based document verification at scale across multiple agencies. The infrastructure is mature. The precedent is established. The only thing missing is the political decision to build it for self-employment.
This framework already exists in law. It is called an Association Health Plan, and it has existed under ERISA for decades. The last serious attempt to expand it happened in 2018, got tangled in court, and has been sitting in regulatory limbo ever since. Both parties have had reasons to keep it small. Neither party has had the political will to unlock it at the scale where it actually works.
Unlock it. Build the federal framework. Build the verification portal. Build the consumer protection floor. And then let the 30 million solopreneurs in this country do what every employer-based worker already does. Stand inside a crowd big enough to get a real price.
Here is what nobody in Washington says out loud.
We say we want to build up small business America. We say we want to encourage entrepreneurship. We put it on campaign posters. Politicians pose for photos in front of bakeries and print shops and mechanic’s garages every election cycle. And then they go back to Washington and leave the healthcare system exactly the way it is.
The harsh reality is that building a small business in this country today takes a level of toughness and grit that most people cannot imagine until they are in it. You will hustle in ways you never thought you would. You will find inner strength you did not know you had. You will carry weight that would break most people, and you will carry it while smiling at clients, paying vendors, making payroll, and pretending everything is fine.
I know. I lived it.
When I was building the pet services business, there were no investors. No fail safe. No runway. I was Ubering. Picking up subcontracted advance work. Taking whatever projects came my way. Building a pet services company including day and night work. Three jobs at once, all of them 1099, all of them real, all of them paying different pieces of the same rent in order to keep a roof over my head. Sleep was for later. Way later.
That is how a seven-figure business that eventually employed dozens of people got started. Not with a funding round. With three 1099s and a refusal to stop.
And through all of it, the health insurance premium was the line item that nearly broke me every single month.
Worth naming while we are here. The gig platforms. Uber. DoorDash. Instacart. Thumbtack. Angi. TaskRabbit. Rover. Handy. Their entire business model depends on classifying workers as 1099 contractors instead of W-2 employees, which saves the platforms roughly 30 percent of what they would otherwise pay in employer-side benefits. Health insurance. Payroll taxes. Workers’ comp. Unemployment. That is not a business model innovation. That is an arbitrage on the backs of the workers. Those platforms have collectively generated hundreds of billions in revenue and tens of billions in profit by routing work to people the platforms refuse to insure. That contribution gap is a separate fight worth having, and that fight is coming in a piece of its own. For now, it is enough to name the pattern. The platforms built the gap. Fixing it is going to require making them help pay for what they stopped contributing when they classified everyone as a contractor.
That is what we are doing to the people we claim to want to encourage. We are telling them we love small business while charging them three times what a cubicle worker pays for the exact same coverage. We are telling them entrepreneurship is the American dream while making the cost of being sick as an entrepreneur financially catastrophic. We are stifling small business America by refusing to fix the one burdensome line item that follows every small business owner from year one through year twenty.
If we actually wanted more small businesses, more entrepreneurs, more builders, we would fix this. The fact that we have not, for five decades, tells you what the people writing the rules actually want.
I would have paid into a national self-employed pool in year one. So would every solopreneur I know. We were never asking for a handout. We were asking for the same pool access that a cubicle worker gets by accident of employment at a large company.
This is not a small fix. It is the single biggest structural change that would help the people who actually built this economy over the last fifteen years. They are not asking for charity. They are asking for fair math.
That is a reasonable ask. And it is already halfway written into federal law.
Fifth: Give the self-employed what Congress already has.
This is the piece that ties the rest of the framework together. And it is simpler than most people realize.
Members of Congress have it. Every federal employee has it. It has been running since 1960. It works. Extend it to the population the system forgot.
It is called the Federal Employees Health Benefits Program. FEHBP. And if you have not heard of it, that is not an accident.
Here is how it actually works. Every federal employee, from a mail carrier to a cabinet secretary, can choose from a menu of plans offered by private insurance carriers. Blue Cross Blue Shield. Kaiser. GEHA. Aetna. The employee pays roughly 25 to 28 percent of the premium out of their paycheck. Taxpayers cover the remaining 72 to 75 percent. The plans are comprehensive. The networks are real. The coverage does not vary by age or health status. Preexisting conditions are irrelevant. Retirees keep their coverage for life if they have been enrolled for at least five years.
FEHBP is why a member of Congress earning $174,000 pays roughly $365 a month for Platinum-level coverage, while the 63-year-old self-employed woman in Florida I wrote about in Part I was quoted $4,923 a month for equivalent coverage. Same country. Same healthcare market. Two completely different pricing structures.
Here is the fix.
Open FEHBP to every self-employed American, every independent contractor, and every gig worker in the country.
Not a replacement for employer insurance. Not a replacement for Medicare, Medicaid, or the VA. An additional track, specifically for the 30 million Americans the current system was never designed to serve.
The private chef booking her own clients. The hairstylist with her own chair. The dog walker with an LLC. The contractor with a truck. The graphic designer with a Shopify site. The consultant running her practice from her kitchen table. The Uber driver, the DoorDash courier, the Rover walker, the TaskRabbit worker. The writer, the therapist, the personal trainer, the real estate agent, the wedding photographer, the bookkeeper, the house cleaner, the handyman, the pet professional, the freelance developer, the plumber running his own shop, the electrician with two employees.
All of them, buying into FEHBP at the same subsidized rate a federal employee pays. Same carriers. Same networks. Same age-neutral, health-status-neutral pricing.
That 63-year-old in Florida goes from $4,923 a month to roughly $365 a month. Same coverage. Same access. Same protection. The only thing that changes is her eligibility.
How this actually pays for itself.
This is where the framework clicks together.
The expansion is funded by the fraud enforcement in Step One. The $200 billion a year in healthcare fraud I walked through earlier is not a theoretical number. It is money already flowing through the system, being stolen in real time. Reclaim a fraction of it. Redirect it to fund the FEHBP subsidy for the expansion population. The math works because the money already exists. It is just currently being captured by bad actors instead of being deployed for the Americans who fund the system with their taxes.
You cannot build this fix in a system that is hemorrhaging fraud. You can build it in a system that has closed the leak. That is why sequence matters.
Verification is already solved.
The portal I described in Step Four handles enrollment. Upload your documentation. AI cross-references against IRS records, payment processor data, and insurance carrier databases. Verification returns in minutes. Schedule C filers, 1099 recipients, LLC owners, S-corp filers, gig platform workers, and active business insurance holders all qualify.
No guild membership required. No industry association. No federal bureaucracy to navigate. Just proof you are self-employed. The federal government already has most of the data. The applicant provides the rest.
What this does not disrupt.
Big corporate keeps its employer-sponsored plans. Nothing changes for the 160 million Americans who get coverage through their job. Their plans stay. Their premiums stay. Their employer contributions stay. If anything, employers benefit, because their contractors, vendors, and freelance collaborators stop leaving projects halfway through due to medical crises.
Medicare stays for seniors. Medicaid stays for low-income Americans. The VA stays for veterans. Tricare stays for military families. The Indian Health Service stays. CHIP stays. Nothing is taken from anyone.
One population gets something they have never had. That is the entire change.
Why this has not already happened.
FEHBP expansion has been proposed by both parties for five decades. Nixon proposed a version in 1974. Ted Kennedy introduced FEHBP-for-all legislation repeatedly. Elizabeth Warren proposed it in 2017. Chris Van Hollen proposed a version in 2019. None of them passed.
The opposition comes from a specific coalition. Individual market insurance brokers, who would lose their commission base. Short-term medical plan carriers, who sell the cheap, limited coverage that FEHBP would outcompete. Pharmacy benefit managers, who profit from the billing opacity that FEHBP would eliminate. A small group of concentrated interests that benefit from the current dysfunction.
The coalition that would benefit is enormous but disorganized. Thirty million self-employed Americans, the small businesses they run, the contractors they hire, the creative economy they power, the gig workforce that keeps the country moving, and every family member connected to them. But these people do not have lobbyists. They do not have a Washington office. They do not have a seat at the table when the legislation gets written.
That is why this fix has been available for 50 years and has not happened.
It is also why this is the fix that is most likely to happen next, if the pressure gets loud enough. Because the opposition is small and self-interested, the beneficiary group is huge, and the infrastructure already exists. There is nothing to build. There is only a door to open.
What gets closed when this opens.
The healthcare penalty on entrepreneurship ends. People who have been afraid to leave a corporate job can start the business they have been dreaming about. The job-lock that suppresses new business formation by roughly 25 percent gets released. The creative class stops being one medical emergency away from bankruptcy.
The age penalty ends. FEHBP does not charge a 63-year-old three times what it charges a 23-year-old. Same coverage, same pricing, regardless of age.
The preexisting condition penalty ends. FEHBP does not underwrite individual risk. Everyone in the pool gets the same access.
The geographic penalty ends. A freelance designer in rural Idaho gets the same FEHBP access as one in San Francisco. Same networks. Same carriers.
The “hope you don’t get sick” penalty ends. Self-employed Americans stop making coverage decisions based on praying nothing happens. They start making coverage decisions based on what actually fits their lives.
The argument that ends the debate.
Members of Congress have FEHBP. They have had it for 65 years. They protect it fiercely. They have voted down every attempt to expand it to the rest of the country while keeping it for themselves.
Every member of Congress who votes against extending FEHBP to the 30 million self-employed Americans who fund the government with their taxes is on record voting to keep a premium benefit for themselves that they will not share with the people who pay for it.
That is not a policy disagreement. That is a two-tier citizenship argument. And once it is named clearly, it does not survive scrutiny.
Give the self-employed what Congress already has. The system is already built. The only thing missing is the will to open the door.
What’s Actually Already in Motion
Here is what is worth sitting with.
The fraud enforcement is already happening. The DOJ numbers are real. The Fusion Center is real. The whistleblower rewards are real. There is political will right now to act meaningfully on one leg of this three-legged problem.
The price transparency rules are already on the books. They are just not being enforced with teeth.
The ACA already contains the interstate compact mechanism. It just was not designed well enough to be used.
Almost everything in the framework I just laid out is either already legal, already authorized, or already underway. What is missing is coordination. Sequencing. The political honesty to tell the country that no single reform is going to fix this and that the ones that work have to be done in the right order.
That is not a policy problem. That is a leadership problem.
Why This Matters
I started this series because of a friend who picked up the phone to say goodbye. I wrote about him in Part I. He is the reason this series exists. He is the face of who the rebuild has to serve.
Not the lobbyists. Not the insurance executives. Not the pharmaceutical CEOs. Not the members of Congress whose healthcare my taxes already pay for.
Him. And everyone like him.
The bartenders who served you dinner last night. The dog walker who took care of your pet this morning. The contractor who fixed your roof last year. The consultant who built your website. The small business owner who employed twelve people through the pandemic and still cannot afford her own health insurance.
The middle. The people who actually keep this country running.
They deserve a system that works. And the reason it does not work is not because the problem is unsolvable. It is because the people in charge of solving it benefit from it being broken.
That is the real gap.
It is not a gap between what we have and what is possible. It is a gap between the people making the rules and the people living under them.
Close that gap and everything else gets easier.
What You Can Do Right Now
Same playbook as Part I and Part II. It still works. It always will.
Run your own numbers. Go to stridehealth.com. Enter your real information. No subsidies. Screenshot what comes back. Then enter 20001, Capitol Hill, and screenshot that. Post both.
Look up your representative at OpenSecrets.org. See who is funding them. Compare that to how they voted on healthcare. The picture tells itself.
Call them. Not email. Call. Congressional offices track call volume. It registers in a way emails do not. Tell them you have been paying attention. Tell them you will continue paying attention.
Vote in every election. The people deciding this are not personally exposed to the consequences. They need to hear from the people who are.
Talk about what you pay. The silence around healthcare costs is part of what keeps the system in place. The moment people start saying the actual numbers out loud, the argument changes.
Share this series. Part I. Part II. Part III. All three. The people in your life who need to read this will not find it on their own.
The system is not broken.
It is working exactly as designed.
The only question left is whether we are willing to change who it works for.
If this landed, share it. Share Part I. Share Part II. Share all three. The people in your life who need to read this won’t find it on their own. Forward it. Post it. Drop it in a group chat.
Not yet a subscriber? Every week, The Jenn Files cuts through the noise on business, money, resilience, and grit — written for people who are building something real. If The Jenn Files is part of how you make sense of the world, consider becoming a paid subscriber. Your support is what keeps this work going.
Prefer to read in the app without the inbox noise? You can switch to app-only notifications in your Substack account settings under Notifications. I want this to work for you however works best.
Sources:
American medical excellence & global dignitary care:
US News & World Report and Newsweek “World’s Best Hospitals” rankings: Mayo Clinic, Cleveland Clinic, Johns Hopkins, Massachusetts General, NYU Langone consistently top international lists
Foreign dignitaries and heads of state seeking care at US academic medical centers: widely documented across major medical institutions
Healthcare spending by country:
US per capita health spending $14,885 (2024): OECD Health Statistics via Health Systems Facts, February 2026
OECD average $5,000 per capita, US 2.5x average: OECD Society at a Glance 2024
Country-by-country spending, coverage, and government share data: OECD Health at a Glance 2023/2025, WHO Global Spending on Health 2024, World Bank
US spends nearly 40% more of GDP than second-place Germany, lowest life expectancy in G7: Economics by Design, February 2026
Fraud enforcement:
2025 National Health Care Fraud Takedown: 324 defendants, $14.6 billion: U.S. Department of Justice, June 30, 2025
Operation Gold Rush: $10.6 billion in fraudulent Medicare claims, one million stolen beneficiary identities: DOJ Press Release, June 2025
Healthcare Fraud Strike Force cumulative: 6,200+ defendants, $45 billion billed since 2007: Skilled Care Journal, 2026
CMS prevented $4 billion ahead of 2025 Takedown: Medical Economics, 2026
DOJ Health Care Fraud Unit $106.76 ROI per $1 spent: Mintz DOJ Year in Review, February 2026
Fraud estimates vs. improper payments:
Over $100 billion in combined Medicare/Medicaid improper payments FY 2023 (43% of all federal improper payments): GAO-24-107487, April 2024
Medicaid improper payments FY 2025: $37.4 billion (6.12%): CMS Improper Payments Fact Sheet, January 2026
Medicare estimated $60 billion/year lost to fraud, errors, abuse: Senior Medicare Patrol
Medicaid improper payments ten-year total $543 billion (CMS) vs. estimated $1.1 trillion (Paragon Institute): CMS Agency Financial Reports; Paragon Health Institute, March 2025
KFF explainer on distinguishing fraud, waste, abuse, and improper payments: KFF, March 2025
Interstate insurance sales:
ACA Section 1333 interstate compacts authorized since 2014: Federal Register, March 2019
Nine states enacted Interstate Health Compact laws; zero compacts formed: Urban Institute
No insurer has sold a policy through any interstate compact mechanism: Georgetown Center on Health Insurance Reforms
Industry and regulator opposition to unrestricted interstate sales: NAIC, American Academy of Actuaries
McCarran-Ferguson Act 1945: SAN.com, December 2025
Universal coverage wait times:
Canada median wait 28.6 weeks, 1.4 million waiting: Fraser Institute, Waiting Your Turn 2025
NHS wait time standards: NHS England, March 2026
Cross-country specialist wait comparison: World Population Review, 2026
VA system:
VA 28-day specialty care access standard: VA.gov Community Care Eligibility
Phoenix VA secret waitlist scandal: Mission Roll Call, 2025
GAO report on VA wait disparities: GAO-25-108101, February 2025
Referenced in Part I and Part II:
Insurance industry lobbying spend $183 million in 2024: OpenSecrets.org
Congressional health insurance taxpayer subsidy 72–75%: OPM, Congress.gov
Pharma/health industry donations: $26.4M Democrats, $16.1M Republicans 2024: OpenSecrets
Rep. Brett Guthrie (R-KY) pharma/health donations: OpenSecrets via Kentucky Lantern, October 2025
One Big Beautiful Bill Act signed July 4, 2025: Brownstein Hyatt Farber Schreck, July 2025
This is Part III of The Gap, a three-part series on what it costs to be in the middle in America right now.